When the 'Unrecognized' Became Essential: How Informal Health Practitioners Helped Vaccinate 58 Zero-Dose Children in Karachi
.JPG.webp)
In some of Karachi’s most vulnerable neighborhoods, the people who ultimately helped children receive their first vaccines were not government vaccinators or public health officials. They were informal private health practitioners, providers who operate small clinics in narrow streets. Critically, the families concerned regarded these health practitioners as their “doctor” of choice.
Our health ecosystem sees these practitioners as outside the formal system. However, our research showed that in resolving protracted issues such as vaccine resistance, their ties of trust to the community could be used innovatively to crack the problem of convincing parents to vaccinate previously unvaccinated children.
The lesson is straightforward but important. Innovative thinking can help resolve protracted attitudinal issues of health behavior that millions of dollars may not be able to. For example, in this case, with trust as the major barrier to vaccinating young children, the catalyst for change is to work through the credible relationships that already exist.
The Immunization Reality in Karachi’s SHRUCs
Karachi is home to over twenty million people. Within its dense urban landscape are Super High Risk Union Councils (SHRUCs) where poverty, overcrowding, and weak public infrastructure shape everyday life. In these areas, zero-dose prevalence (i.e. children who have received none of their mandated vaccinations) is around 10.3%. This reflects more than service gaps. It reflects the disconnection of segments of society from the health system itself.
Vaccines are available. Public facilities exist. Yet many children miss even the first dose of Penta-1, which serves as the entry point into routine immunization. Why is this so, and what can be done about it? That was the question our research attempted to answer.
Understanding Behavior Through Research
The “Zero Dose Learning Agenda” project in Karachi attempted to investigate the issue of unvaccinated children, beginning with a critical question. Why are caregivers still disconnected from routine immunization despite physical access to services?
A mixed-methods approach grounded in what is known as the “Intent, Access, and Readiness” framework combined secondary data analysis, geospatial mapping, qualitative interviews, focus group discussions, and Human-Centered Design workshops across the Union Councils of Islamia Colony, Muslimabad, and Mangopir to help answer this question.

Image 1: ZDLA HCD Workshop with caregivers, Islamia Colony.
Trust, Not Distance, Was the Barrier
Research showed vaccination sites were geographically accessible, and system readiness was largely decent. However, caregivers described long wait times, negative staff attitudes, concerns about medicine quality, and mistrust of public facilities as anchoring points in their thoughts about the public health system (Figure 1). Clearly, the primary issue that needed to be resolved was not access, but trust when trying to convince parents to vaccinate unvaccinated children, and that trust was unlikely to be built in the public facilities that provided a poor patient experience.
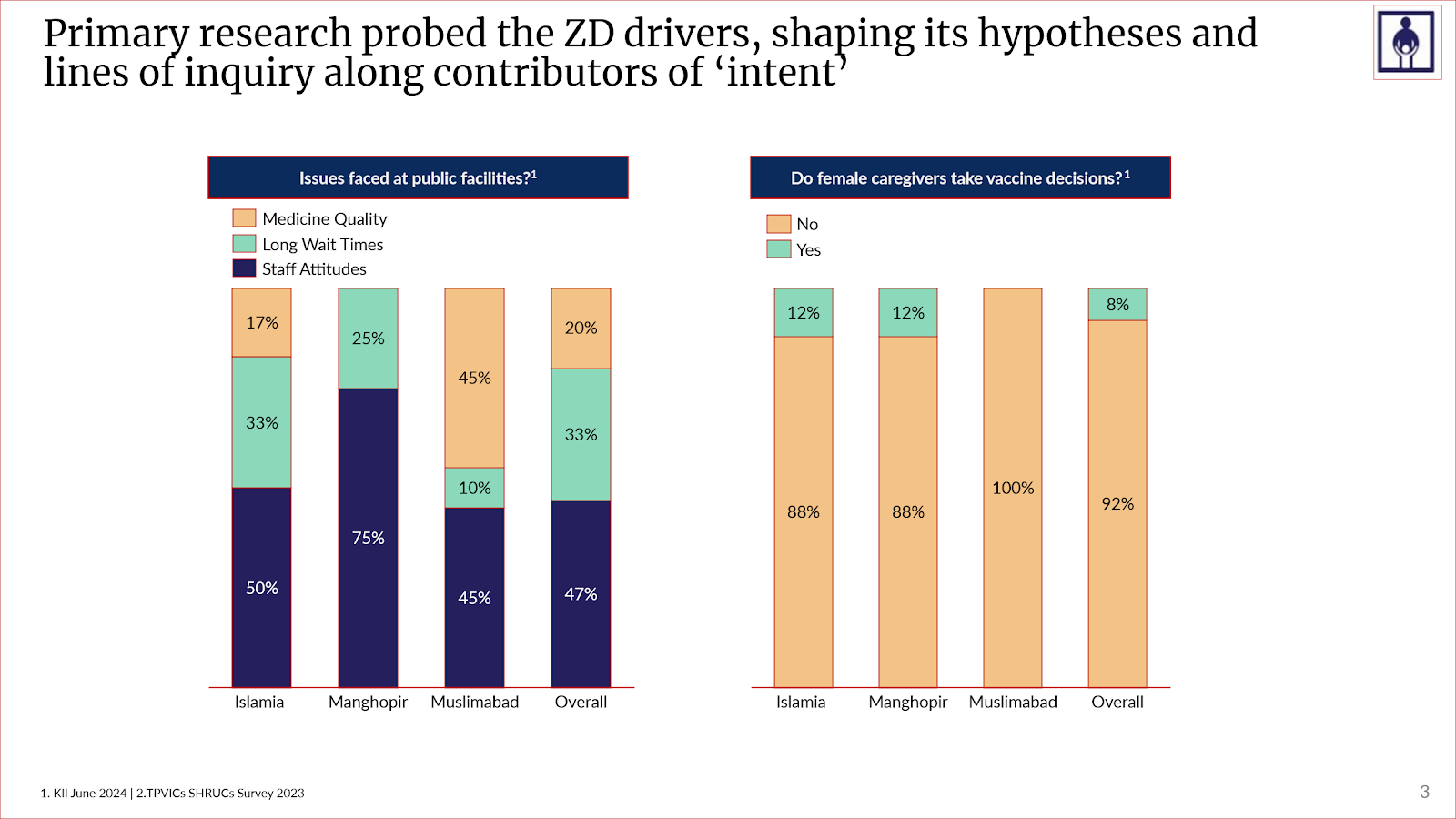
Figure 1: Primary research with caregivers
Designing with Reality, Not Against It
Informal practitioners were identified as trusted first points of care. Rather than replacing them, our research considered them as behavioral gatekeepers who could counsel caregivers and refer eligible children to nearby public vaccination sites.
A referral slip system and closed-loop verification linked to the Sindh Electronic Immunization Registry ensured accountability and follow-up.

Image 2: ZDLA team member providing training to a private practitioner in Islamia Colony.
Converting Trust into Action
Between February and October 2025, our team trained 11 informal practitioners on counselling parents on the importance of vaccinations available at public healthcare facilities. The practitioners counselled 589 children, of whom 119 were verified as vaccinated, including conversions of 58 zero dose children. Exit surveys showed increased understanding, reduced fear, and stronger confidence in vaccination decisions following practitioner counselling.
This experience shows that as governments and donors think about challenging issues such as vaccine resistance, they need to think outside the box. Improving primary healthcare indicators cannot only be about forever expanding access through infrastructure that works poorly, but about building trust in communities to be able to use the infrastructure already in place. When trust is weak, even a short distance can feel far. In this case, that trust in the importance of vaccination can be built by having thought through who in the community is best placed to convince mothers to vaccinate children, and to use them, even if they lie outside of the formal healthcare system.



